Rectal bleeding - causes, diagnosis and treatment
Rectal bleeding, also known as rectal bleeding, is a symptom that requires careful analysis and clinical interpretation, considering the wide range of potential causes.
Diagnostically, identifying the source of bleeding requires a thorough analysis, taking into account factors such as the duration and characteristics of the bleeding, the presence of accompanying symptoms (pain, changes in bowel habits, weight loss), and medical history and risk factors. Diagnostic methods such as proctoscopy, colonoscopy, or digital rectal examination are essential for visualizing pathological changes and, if necessary, collecting specimens for histopathological examination.
Causes of rectal bleeding
Rectal bleeding can be caused by a variety of health conditions. Common causes include hemorrhoids, anal fissures, inflammatory bowel disease, intestinal polyps, and gastrointestinal infections. Less commonly, it can be a symptom of more serious conditions such as Crohn's disease, ulcerative colitis, or colon cancer.
This symptom may be a manifestation of pathological conditions such as hemorrhoids or anal mucosal fissures, or indicate more complex and potentially dangerous diseases, including colon cancer, inflammatory bowel disease or adenomatous polyps.
Symptoms associated with rectal bleeding
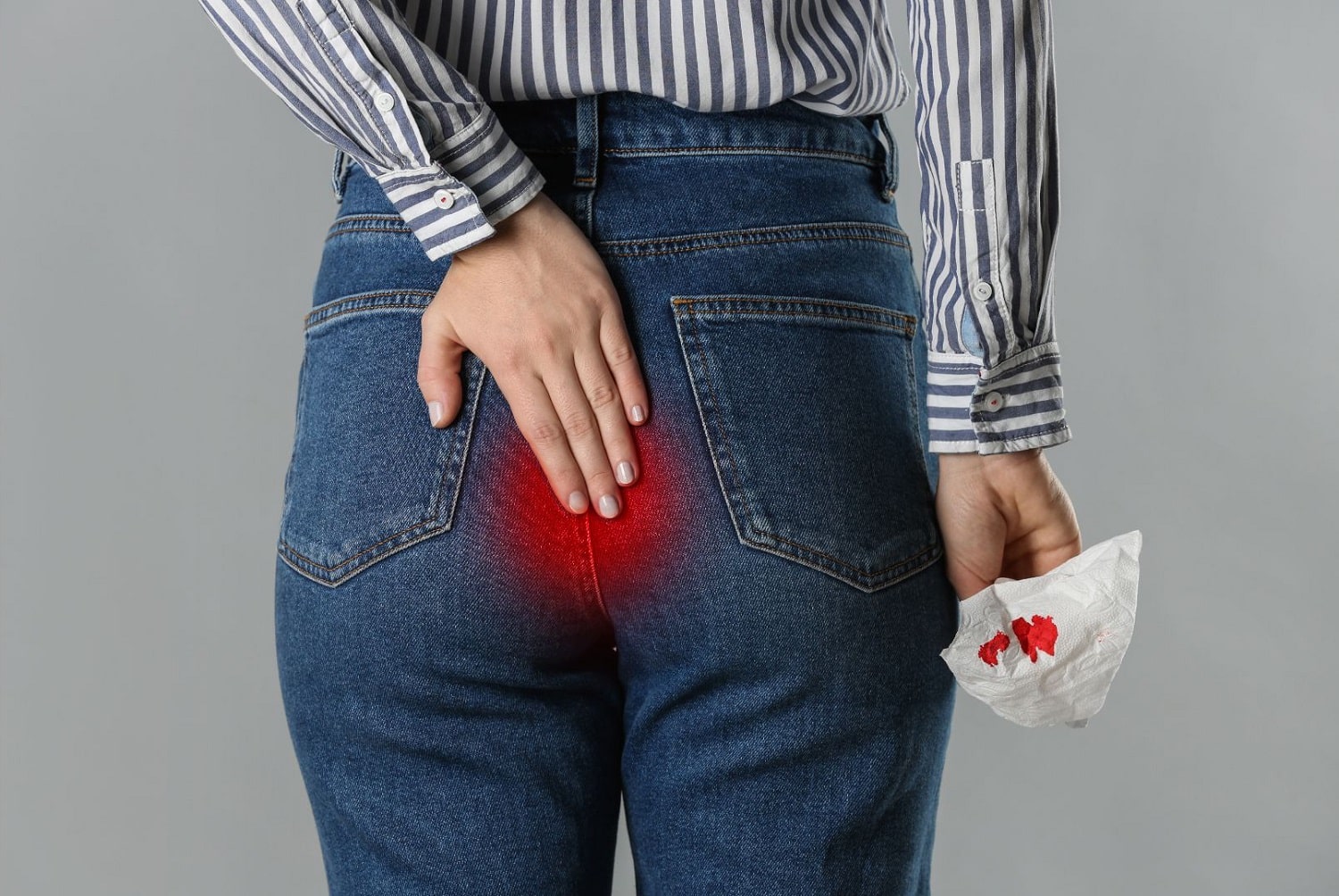
Rectal bleeding is blood loss through the rectum , which may be noticeable as blood on toilet paper, in stools, or in the toilet after a bowel movement. It can range in intensity from light streaking to heavy bleeding.
In addition to bleeding, other symptoms may include pain or discomfort around the anus, changes in bowel habits, changes in stool appearance, a feeling of incomplete evacuation, and general symptoms such as weakness or weight loss. It's important to note the nature of the bleeding and other accompanying symptoms.
Rectal bleeding and hemorrhoids
Rectal bleeding is one of the most common symptoms of hemorrhoids, a condition characterized by dilated and inflamed veins in the anal canal and lower rectum. Hemorrhoids are classified as internal, located above the anal dentate line, and external, located below this line. Bleeding, usually painless, may occur during or immediately after a bowel movement, for example, on toilet paper.
The mechanism of bleeding in hemorrhoids involves damage or rupture of the hemorrhoidal surfaces, which can occur as a result of increased internal pressure within the anal canal. This pressure can result from chronic constipation, prolonged sitting, pregnancy, excessive straining during defecation, and other predisposing factors.
Diagnosis of hemorrhoids is primarily based on a proctological examination, including inspection of the anal area, palpation, and anoscopy, which allows for a thorough assessment of the internal structures of the anal canal. If the diagnosis is unclear or if bleeding persists despite treatment, additional tests, such as a colonoscopy, may be recommended to rule out other causes of bleeding, including inflammatory bowel disease or cancer.
Diagnosis and treatment
Diagnosis of rectal bleeding may include a proctological examination, colonoscopy, blood tests, and in some cases, imaging tests such as computed tomography (CT) scan. Treatment depends on the cause of the bleeding and may include dietary changes, medications (e.g., anti-inflammatory, hemostatic), and in some cases, surgery.
When to consult a doctor?
Consultation with a doctor is recommended in several cases. This is especially true if rectal bleeding is heavy, recurring, or accompanied by other disturbing symptoms such as pain, changes in bowel habits, weight loss, or general weakness. If any rectal bleeding occurs, especially in people over 50 years of age or with a family history of intestinal disease or cancer, you should consult a doctor immediately.